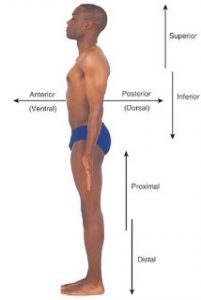
What is Range of Motion? The normal movement of joints.
For many residents, a lack of mobility causes stiffness in their joints. Their muscles shrink and become weak- this is known as atrophy. Gradually, the atrophied muscles become hard and rigid. The muscles shorten in this process, and therefore joint movement is affected. Pain, discomfort and disfigurement occur. These disfigurements are known as contractures. They are, almost always, 100% preventable.

To be effective, ROM exercises should be performed at least twice a day, and each exercise should be done at least five times. The quick, natural opportunities for ROM are an excellent way to enhance what we do, but it should never replace a full program. The only way to fully perform all the exercises, is during AM/PM cares, with a complete focus on this one activity.
Some residents will be able to help. They can move their joints without our help-this is called ACTIVE RANGE OF MOTION. The resident can perform almost all the exercises on their own, through a dedicated program or through normal activities of daily living.
Other residents can perform SOME portion of ROM, but due to weakness, pain, paralysis and the like, they will need limited amounts of assistance. Usually they can tell you exactly what you need to do. This is called ACTIVE ASSISTED ROM.
For most of the residents we deal with, PASSIVE ROM is the norm. These residents cannot assist with this, for many reasons. It’s important to remember that these ROM exercises do not strengthen the muscles; they prevent deformity and maintain movement.
A great way to make ROM a part of AM/PM care might include applying lotion to those body parts being exercised. The lotion is calming and relaxing, and this will help with ROM. Another good time is during a bath. If you note the resident experiences pain during ROM, ask the nurse about pain medications being given 30 minutes or so before the exercises are started.
If ROM is problematic to complete due to time restraints, ask your co workers if they too are having trouble. As a group, you all could seek ways to help each other. Or, seek the advise of the charge nurses. At one nursing home I know of, the aides simply did not have time to complete ALL the ROM for each resident. The aides met with the nurses, who went to the DON to get some ideas and guidance. The DON met with the Activity Director, who implemented an exercise activity designed to provide ROM to those residents the aides could not get to in the morning. The aides marked off who received ROM and who didn’t, and the Activity Staff provided the exercises as part of special “Massages” and other aptly titled programs.
Another nursing home I know of breaks up the ROM requirements for each shift. This means third shift does some of these programs- especially for those residents who are awake during their shift.
Creative minds can ensure that vital care is provided. Dedicate TIME for this very important skill…this task…this care. ROM should not be skimped on, ever.